First of all, let me start by saying thank you. I thank you for all the calls and emails. I do apologize for not being so good at getting back to you. I do have an explanation, and I hope you will indulge me a bit and read a bit further. I promise it is not your standard the-dog-ate-my-cell-phone excuse.
I also wanted to take a few moments to write down all of my thoughts and information in one place. I want people to be able to read my words, so there is no confusion about what this is or isn’t.
I hope that by telling about my experiences, I will help inform at least one person (or a dozen :) about Cushing's. I've included some resources that it has taken me over a year to find. I put it in one place to make things easier: photos, diagrams, videos, articles, etc. The videos on the left navigation bar are fascinating and very informative. I hope you will stick around and check things out. ~Melissa
*******
As you know, I moved with my fiancé Jonathan to San Antonio in November 2006 for a job opportunity for him. I took some time off post election as we moved into our first home, geared up the wedding planning, and tried to enjoy the holidays. Very quickly, however, I realized something was wrong with me. I didn’t feel like myself. For the next four to five months, I was stressed still, confused, crying a lot, feeling depressed, posting high blood pressure, gaining a lot of weight, and missing menstrual periods (2nd time in 14 months where I missed 4 periods in a row). I had terrible pains in my whole body, muscles and legs. I was a mess. Thinking all the wedding planning stress was the culprit, we decided to move the wedding from April to October 2007.
A few months later, there was really no relief from my symptoms. In March 2007, I went to my primary care doctor who checked my thyroid levels. The tests came back normal. The doctor was nice but didn’t have any concern to continue to test me. I cried. I knew there was something wrong with me. I was determined to find out what it is. I took to the internet and within an hour I found my answer.
I will never forget that day: March 28, 2007 at 4:53 pm. A quick research of my symptoms brought me devastating news.
I suspected that I had Cushing’s disease. Nine months, $100,000 in medical bills (our portion was only $4,000), and countless doctor visits, two MRIs, tubes of blood for lab work, and more tenacity than I knew I had got me to the end. On December 20, 2007, I would finally hear my San Antonio neurosurgeon give that same diagnosis: Cushing’s disease.
My endocrinologist says that Cushing’s is the most difficult diagnosis in the field of endocrinology if not all of medicine.
Leave it to me to be so extraordinary!
I am devoting this blog to create awareness for Cushing’s disease. It is my little attempt to shed light on this disease by sharing my own struggles and experiences on the path to diagnosis and, eventually, surgery.
I hope you will take a moment to read further.
Cushing’s is underdiagnosed because so many of its symptoms overlap with other, more common diseases. Doctors treat those diseases while telling us that Cushing’s is far too rare for us to actually have. The doctors-turned-mathematicians tell us that it is nearly statistically impossible for us to have Cushing’s. Yet, patient after patient have proven them wrong—through pathology confirmation at surgery—but there is still many more doctors and patients to reach out there.
********
WHAT IS CUSHING’ DISEASE?
Cushing’s disease is a very rare disease that affects an estimated 10 to 15 people per million per year, or about 3,500 people per year in the US alone. Those of us with this disease feel like this number grossly underestimates how many undiagnosed people there are.
Cushing's disease affects women five times more frequently than men.
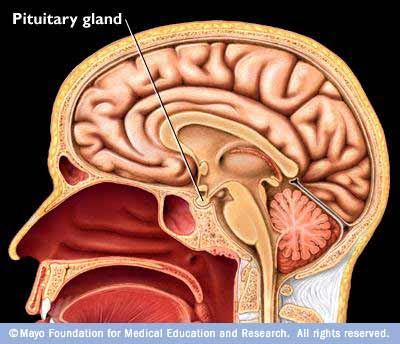
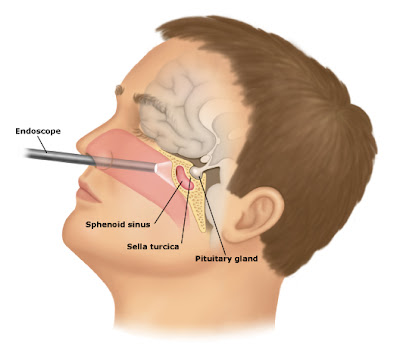
Cushing’s disease caused by a benign tumor located on the pituitary gland, the little bean size gland hangs just below the brain. Named the “master gland,” the pituitary gland controls every hormonal process in the body.
These tumors are benign, or non-cancerous, tumors of the pituitary gland secrete increased amounts of ACTH. Most patients have a single adenoma. After two brain/pituitary MRIs and consults with two different neurosurgeons, we now know that I have two pituitary tumors: a 5 millimeter tumor on the right side and a 3-millimeter tumor on the left side. While small—teeny tiny most would say—these little buggers are wreaking hormonal havoc on my body. Even a tumor of one cell can cause major upheaval to a person’s hormonal balance.
WHAT DOES CORTISOL DO FOR THE BODY?
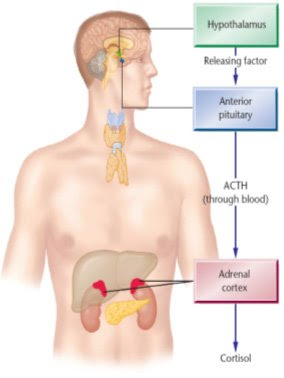
Cortisol performs vital tasks in the body. It helps maintain blood pressure and cardiovascular function, reduces the immune system's inflammatory response, balances the effects of insulin in breaking down sugar for energy, and regulates the metabolism of proteins, carbohydrates, and fats. One of cortisol's most important jobs is to help the body respond to stress. For this reason, women in their last 3 months of pregnancy and highly trained athletes normally have high levels of the hormone.
When the amount of cortisol in the blood is adequate, the hypothalamus and pituitary release less CRH and ACTH. This ensures that the amount of cortisol released by the adrenal glands is precisely balanced to meet the body's daily needs. However, if something goes wrong with the adrenals or their regulating switches in the pituitary gland or the hypothalamus, cortisol production can go awry.
SYMPTOMS ASSOCIATED WITH CUSHING’S DISEASE
- Rounding of the face (moon face)
- Facial redness (facial plethora or red cheeks)
- Acne
- Hump on back of neck (dorsocervical fat deposition), called a buffalo hump
- Weight gain around the belly with thinner arms and legs (truncal obesity) despite efforts to lose weight (lifestyle modifications)
- Pink or purple stretch marks (striae) on the skin of your abdomen, thighs, breasts and arms
- Thicker or more visible body and facial hair (hirsutism)
- Muscle weakness
- Extreme fatigue
- Thin and fragile skin that bruises easily
- Slow healing of cuts, insect bites and infections
- Bone thinning (recurrent fractures, osteoporosis)
- Recurrent infections
- Sleep disturbances (waking in the middle of the night)
- High blood pressure
- Diabetes mellitus
- Depression, anxiety, crying, and irritability
- Confusion, mind fog, slowed memory
- Low self-esteem
- Irregular or absent menstrual periods in females
- Decreased sex drive
When I read this list of symptoms, I couldn't believe myself. I knew I had just diagnosed myself. I was in shock. I was amazed. I had to wait over an hour before Jonathan came home from work. I remember that I waited for him to enter the house. I gave him a hug, and then I said, "I think I have Cushing's disease, and if it is, there is a 70% chance I have a tumor in my brain or pituitary." He of course was shocked too.
Not only did I experience nearly all of the symptoms on the list, I knew when I read the words "buffalo hump" that this was it. I just knew this is what I had.
Here is the buffalo hump picture I saw on the internet:


Here is my buffalo hump.


I searched the internet to see what else could cause a buffalo hump.
- Cushing's disease
- Long term use of steroids
- Morbid obesity
- AIDS medications
- Kyphosis
- Pituitary tumor
- Hyperinsulinaemia
I looked up all the unfamiliar terms, and I knew they didn't apply. It could only be Cushing's.
I set up an appointment to see a doctor that was listed as an endocrinologist in San Antonio who understood Cushing's. However, I couldn't get in to see him until May 9th.
So for the next six weeks, I researched. I read. I cried. It was so painful to watch my body get worse. The waiting was awful. I noticed weight gain, sleep loss and a sudden personality change. I felt like my life was spiraling downward. I recorded 40+ symptoms in a journal to monitor patterns in my illness.
I didn't feel like myself, and I remember the probability lessons from my math classes. If I only had a few symptoms from the above list, I couldn't say with much probability that it was Cushing's. But as my list of symptoms and health complaints mirrored nearly every one of the symptoms for Cushing's, I knew it made the diagnosis of Cushing's even more probable--and very improbable that it could be several other diseases all happening at the same time. A doctor later confessed that doctors are taught to find one diagnosis that fits the slate of symptoms. However, because doctors believe Cushing's is so rare and improbable, they often treat the symptoms. As a result, the patient rarely improves and years pass before the patient gets the help s/he needs and deserves.So I pushed forward, sought out information and specialists, all trying to see if I had indeed diagnosed myself. If not, I was prepared for someone to tell me what else it could be. As the days and months passed, doctors scratched their heads about my high cortisol and ACTH test results but yet hesitant to say for sure that it was Cushing's.
I always knew. And I will always be happy to say that, I was right. Even with news this devastating, it was important to finally know what ailed me. To my dying day, I will always be proud of my ability to trust my instincts and move forward despite all that I faced. :)
LONG TERM COMPLICATIONS FROM CUSHING’S
If you don't receive prompt treatment for Cushing's syndrome, other complications may occur, such as:
- Bone loss (osteoporosis), due to the damaging effects of excess cortisol
- High blood pressure (hypertension)
- Kidney stones
- Diabetes
- Unusual infections (some patients suffer from boils)
Luckily, I caught my case of Cushing's early enough that I don't have any of these long term complications. Unfortunately, I know many ladies and gentlemen who have these and are still struggling with doctors to get diagnosed. Over the years, the body becomes debilitated by the overproduction of cortisol, and the body's systems are compromised.